- HOME
- VENUE
- RSVP
- REGISTRY
- CONTACT
- Replay media catcher registration code
- Youtube chirp programming
- Kali install pip3
- Motor heavy truck service manual
- Does medicare cover accu-chek test strips
- Always bon jovi backing track
- Ilayaraja instrumental mp3 buy online
- Dead space 2 multiplayer
- New dj mix 2021
- Yamaha mio sporty specs
- Ecm finance
- Do you get viruses for the fortnite downlaod
- Is nero 12 platinum compatible with windows 10
- 1917 german mauser rifle
Aetna considers glucose test strips included on the Formulary Exclusions List to be medically necessary for those members who meet ANY of the following criteria:Ī. All glucose test strips except Onetouch Ultra Test Strips, Onetouch FastTake Test Strips, Onetouch SureStep, Onetouch Verio, Freestyle Test Strips, Freestyle Lite Test Strips, Freestyle Insulinx Strips, Precision Xtra Test Strips, or Precision Xtra Ketone Strips are excluded from coverage for members enrolled in prescription drug benefit plans that use a closed formulary, unless a medical exception is granted. (See Medical Exception Criteria below).Īll glucose test strips except Onetouch Ultra Test Strips, Onetouch FastTake Test Strips, Onetouch SureStep, Onetouch Verio, Freestyle Test Strips, Freestyle Lite Test Strips, Freestyle Insulinx Strips, Precision Xtra Test Strips, or Precision Xtra Ketone Strips are currently listed on the Aetna Formulary Exclusions List and Step-Therapy lists. If it is medically necessary for a member to be treated initially with a medication subject to step-therapy, the member, a person appointed to manage the member’s care, or the member's treating physician may contact the Aetna Pharmacy Management Precertification Unit to request coverage as a medical exception at 1-80.
#Does medicare cover accu chek test strips trial#
Aetna considers All glucose test strips except Onetouch Ultra Test Strips, Onetouch FastTake Test Strips, Onetouch SureStep, Onetouch Verio, Freestyle Test Strips, Freestyle Lite Test Strips, Freestyle Insulinx Strips, Precision Xtra Test Strips, or Precision Xtra Ketone Strips to be medically necessary for those members who meet the following step-therapy criteria:Ī documented trial of one month each of two of the preferred alternative test strips Onetouch Ultra Test Strips, Onetouch FastTake Test Strips, Onetouch SureStep, Onetouch Verio, Freestyle Test Strips, Freestyle Lite Test Strips, Freestyle Inulinx Strips, Precision Xtra Test Strips, or Precision Xtra Ketone Strips

Under some plans, including plans that use an open or closed formulary, All glucose test strips except Onetouch Ultra Test Strips, Onetouch FastTake Test Strips, Onetouch SureStep, Onetouch Verio, Freestyle Test Strips, Freestyle Lite Test Strips, Freestyle Insulinx Strips, Precision Xtra Test Strips, or Precision Xtra Ketone Strips are subject to step-therapy. If precertification requirements apply, Aetna considers these drugs to be medically necessary for those members who meet the following precertification criteria:Īll blood glucose test strips are subject to a quantity limit of 300 test strips per 30 days or 900 test strips per 90 days. Under some plans, including plans that use an open or closed formulary, all blood glucose test strips are subject to precertification. Medicare won’t pay claims for doctors or suppliers who aren’t enrolled in Medicare.Onetouch Ultra Test Strips, Onetouch FastTake Test Strips, Onetouch SureStep, Onetouch Verioįreestyle Test Strips, Freestyle Lite Test Strips, Freestyle Insulinx Strips, Precision Xtra Test Strips, Precision Xtra Ketone Strips If suppliers aren’t participating and don’t accept assignment, there’s no limit on the amount they can charge you.
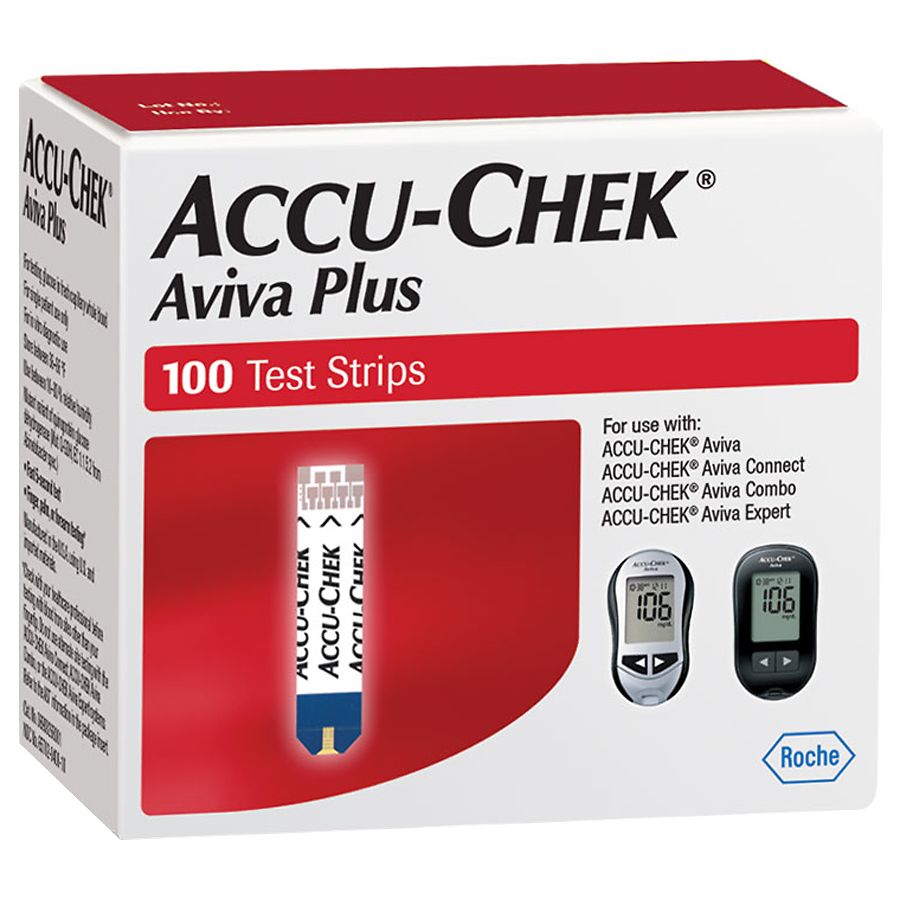
If suppliers are participating suppliers, they must accept assignment (which means, they can charge you only the coinsurance and Part B deductible for the Medicare‑approved amount). It’s important to ask your suppliers if they participate in Medicare before you get DME. Make sure your doctors and DME suppliers are enrolled in Medicare.

If your doctors or suppliers aren’t enrolled, Medicare won’t pay the claims submitted by them. Doctors and suppliers have to meet strict standards to enroll and stay enrolled in Medicare. Medicare will only cover your DME if your doctors and DME suppliers are enrolled in Medicare.

Medicare pays for different kinds of DME in different ways. You pay 20% of the Medicare-Approved AmountĪpplies.